
What happens in residential aged care – and what do residents think?
Following years of criticism about the state of the Australian residential aged care system, including a Royal Commission, the Australian Institute for Health and Welfare has released the results of the latest National Mandatory Quality Indicator Program (QI Program), expanded since July 2021 to include the categories of pressure injuries, physical restraint, and unplanned weight loss.
The fourth quarterly report (April-June 2022) of the GEN Aged Care Data shows that -
- Pressure Injuries in residential aged care affected 6.3% of residents
- Physical Restraint was used for 21.5% of care recipients
- Significant Unplanned Weight Loss was observed in 9.4% of residents
- Falls (32.2% of residents) and falls that resulted in major injury (2.2%)
- Details
Read more: What happens in residential aged care – and what do residents think?

Dementia becomes Australia’s second leading killer
Dementia has become the second leading cause of death in Australia, according to the latest figures from the Australian Institute of Health and Welfare (AIHW), which has recorded a total of 14,464 deaths attributable to the disease in 2020, up from 9200 in the 2010 year.
Dementia is a general term for loss of memory, language, problem-solving and other thinking abilities that are severe enough to interfere with daily life. Alzheimer’s is the most common cause of dementia.
- Details
Read more: Dementia becomes Australia’s second leading killer

Andrew Binns - a life in service
Andrew Frederick Binns was born and raised in Adelaide. He is the youngest of four children to Margaret Dickson and psychiatrist Dr Raymond Binns.
He attended Prince Alfred College, a boy’s school in Adelaide. Even as a teenager, he was a mover and shaker, and argued for ballet to be introduced as a school sport. In this he was successful and his sister staged the choreography. The star of the show John Tilbrook went on to prominence in that other “aerial ballet”, first with Sturt in the SANFL before transferring to the Daemons in the VFL in 1971.
Andrew received a BSc at the University of Adelaide before completing his medical degree at the University of NSW. His early post graduate years were spent at Royal Adelaide hospital and Adelaide Children's Hospital. In 1976 together with his new wife, Jeni, he took the dangerous but fascinating overland route to the UK via Nepal, Afghanistan and the Middle East. It was a cultural experience in both a social and gastroenterological sense.
In England he was a senior house officer in anaesthetics and obstetrics at Upton Hospital, Slough and City Hospital, Nottingham obtaining his diploma in both these fields. He returned to Australia in 1979 settling on the Northern Rivers.
- Details
- Written by: David Guest
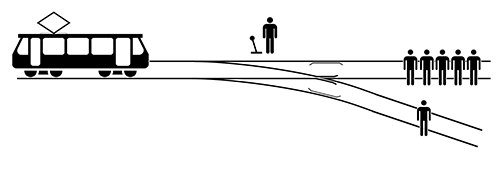
The Trolley Problem
- Handbook of Robotics, 56th Edition, 2058 A.D."
- A robot may not injure a human being or, through inaction, allow a human being to come to harm.
- A robot must obey the orders given it by human beings except where such orders would conflict with the First Law.
- A robot must protect its own existence as long as such protection does not conflict with the First or Second Law.
The laws were first promulgated by science fiction writer Isaac Asimov in 1942 for his short story “Runaround”. In that story Robot SPD-13, “Speedy” becomes paralysed trying to resolve conflicts induced by trying to obey both the second and third laws.
In the spirit of binary computing Assimov later added an additional law. The Zeroth Law states, “A robot may not harm humanity, or, by inaction, allow humanity to come to harm”. Following the structure of the other laws it is taken to be pre-eminent.
However, the addition of the zeroth law leads to unresolvable dilemmas as a robotic variant of the philosophical conundrum, “The trolley problem”.
- Details
- Written by: David Guest

One Curious Doctor - Hilton Koppe
Dr Hilton Koppe reflects on his recently published memoir.
One Curious Doctor is a collection of short pieces born out of my experiences working as a GP in the Northern Rivers since 1988. It also includes stories which have their roots in my personal journey as a migrant growing up in 1960s Sydney, as the descendent of grandparents forced to escape Europe to survive, and as the son of parents who died prematurely from conditions that modern medicine could not cure.
In 2019, these worlds collided. I was diagnosed with Post Traumatic Stress Disorder. I received this diagnosis both as a shock - This can't be happening to me. I'm a doctor. Not a patient! And as a gift - Does this mean I actually get to rest now?
As the fallout from the trauma of the diagnosis began to settle, I tried to work out how I ended up in this position.
- Details
- Written by: Dr Hilton Koppe
Page 12 of 177















